- Controversial issues that affect the dental implant dentistry
Analysis Of The Shortcomings Of Straumann's® BLX/TLX Implant System
- Gerald Niznick
Straumann claims BLX/TLX implants are “Fully Tapered”. In fact, they are straight for the top 12mm with an extremely tapered inner core that creates space for bone chips.

Spiral, bi-directional “claw-like” grooves create bone chips > deposited at the recesses of the deep threads and sluiceways, rather than condense bone

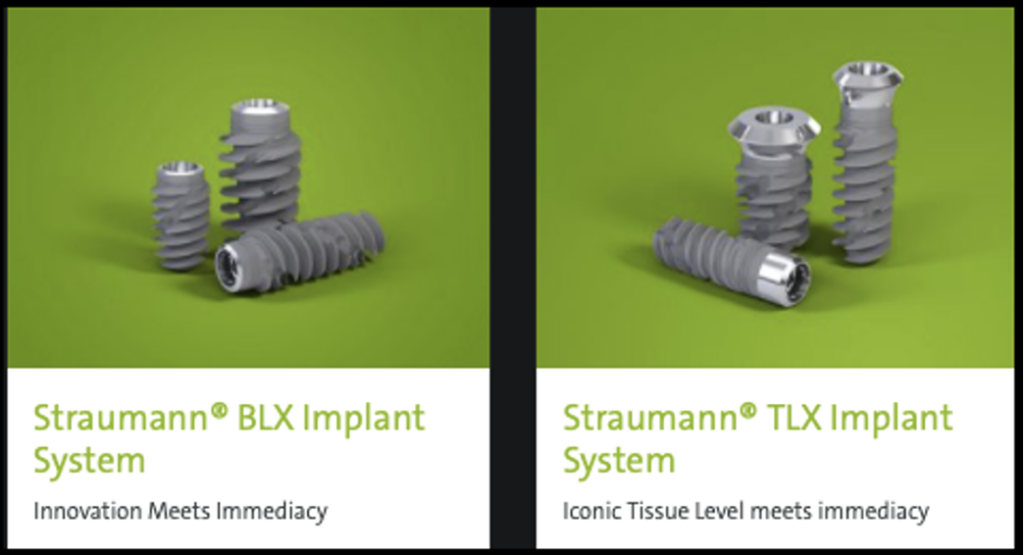
Straumann’s flagship product line is now the BLX (Bone Level) and TLX (Tissue Level) implants with only 1-3 years of clinical documentation. Both have the same thread design and a 7-degree internal connection, called TorcFit. The BLX is a traditional bone-level implant with a blasted surface to the top, while the TLX has a 1.8mm or 2.8mm smooth neck. Both implants are straight for the first 12mm with a tapered core so that the threads get deeper toward the apex. Both have spiral, bi-directional cutting grooves designed to “cut, distribute, collect and condense” the bone chips created by the “lion’s claw-like” cutting grooves. It is a well-established principal that inserting a tapered implant into an undersized socket in soft bone increases stability.
1. Inserting a straight implant into an undersized socket risks a fracture of the bone
2. Rather than condense bone for increased stability, these implants turn bone into chips and collect these chips between the deep threads and cutting grooves. Condensing bone increases initial stability whereas turning cortical bone into bone chips does not.
3. Having a single diameter internal connection for 7 diameters of implants, limits the ability to create a natural emergence profile. Wider abutments that overlapping the shoulder of the implant are available for the 3 widest BLX implants. This defeats the advantages of the frictional retention of the implant’s internal conical connection, thereby increasing the chance of screw loosening.

MISCONCEPTION #1: Straumann’s SLActive surface treatment reduces healing time by 50% Straumann claims its SLActive Surface Technology “Accelerates Osseointegration [for] Reduced Healing Time….You can reduce your patients’ healing time by 50%.” A review of the studies relied on by Straumann do not support its claim that SLActive surface “reduces healing time by 50%”. On their face, these claims are suspect because they do not say 50% faster than what. These claim comes from studies by Straumann’s paid opinion leaders over a decade ago, who merely loaded the SLActive implants at 4 weeks compared to the then recommenced 8 weeks. When the implants still achieved Osseointegration, they claimed the surface was responsible for cutting the healing time in half, when all the study did was cut the loading time
Straumann charges $479 for the BLX implant with the SLA surface while charging $535 for the same implant with its “hydrophic” SLActive surface. The difference in packaging the same implant in a sterile saline solution may cost a few dollars more in contrast to the $56 more Straumann is charging for the more expensive packaging.
A 2021 study in JOI Vol. 47, Issue 2 concluded: “The present study demonstrated that dental implants provided with a hydrophilic moderately roughed surface….did not show any significant improvement of primary or secondary stability compared with implants provided with a hydrophobic surface”

MISCONCEPTION #2: Roxolid is stronger than Ti6AL4V used by most manufacturers. Straumann’s implants are made from an alloy of Titanium and Zirconium. Most other implant companies use Ti6Al4V which has a modulus of elasticity more than twice that of Ti16Zr and therefore, is less brittle.
“Young’s modulus is a measure of the ability of a material to withstand changes in length when under lengthwise tension or compression. Sometimes referred to as the modulus of elasticity, Young’s modulus is equal to the longitudinal stress divided by the strain.”

MISCONCEPTION #3: Using only one connection “simplifies workflow”. Straumann claims that by using only one connection for all the diameters of BLX and TLX implants, they have “Simplified Workflow [and] Reduced inventory.” While it is true that only having one connection would reduce the inventory of abutment and transfer components, this has nothing to do with a “Simplified Workflow.” Color-coded platforms and prosthetic components, as well as All-in-1 packaging, simplifies workflow.

MISCONCEPTION #4: Using only one connection to reduce inventory is worth the compromise of not being able to achieve an esthetic and hygienic emergence profile. The major shortcoming of having only one connection for 7 diameters is the unaesthetic and unhygienic emergence profile that is created when using abutments that fit into the conical connection of wider implants, leaving the implant’s shoulder exposed.
MISCONCEPTION #5: Straumann can overcome the BLX’s emergence profile problem by offering abutments that sit on the shoulder of the implant.
Straumann offers a wider abutment option for the 3 widest implants, that seats on part of the implant’s shoulder. Straumann claims its TorcFit is a hybrid connection that can interface with either the internal 7 degree cone or the shoulder of the implant. As shown below, the wider abutments only make contact on its periphery. Abutments that seat on the top of the implant cannot also engage the internal conical connection, sacrificing stability for a better emergence profile. Paragon’s new conical connection includes a deeper Morse Taper connection for a friction-fit even when the abutment seats on the top of the implant.

MISCONCEPTION #6: Having the neck of the implant narrower than the thread diameter reduces stress at the crest of the ridge. The thread diameter of the wider implants is greater than the diameter of the neck of the implant. That difference increases with the wider implants. Straumann claims the narrow neck reduces stress at the crest. What it does in actuality, is reduce stability because of the lack of contact near the crest. It also leaves a gap at the crest of the ridge that could encourage soft tissue downgrowth.
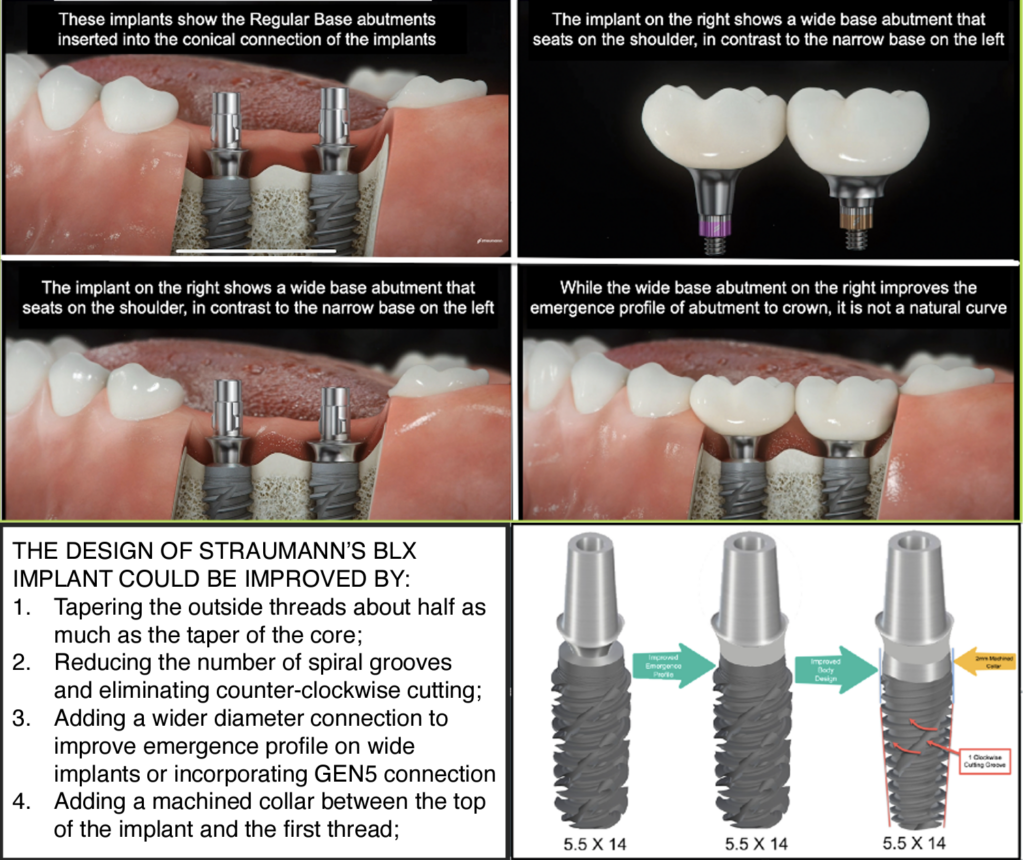
MISCONCEPTION #7: Straumann claims the BLX’s fully tapered core “allows for insertion into a small and undersized osteotomy”. The BLX Implants are basically straight with only a slight reduction in diameter to the outside thread diameter below the top 12mm. Forcing a wide apex of an implant into an undersized socket increases the risk of bone fracture and may cause the implant to not fully seat, even when using the widest drills recommended for dense bone. BLX’s final seating in dense bone may require the reverse cutting grooves to enlarge the site by turning more bone into bone chips. This video shows that for a 4.5mmD implant, final sizing with a 4.2mmD drill may not be enough bone reduction to fully seat the implant. The concept of inserting a tapered implant into an undersized socket was first explained in a 1995 patent (Niznick U.S Pat #5,427,527) and documented in a 2000 Niznick Journal Article. This picture compares the apex of a 4.7mm X 13 mm tapered GEN5™ to a 4.5mm X 12mm BLX. The GEN5™’s apex could start more easily into an undersized socket.

MISCONCEPTION #8 & 9: The BLX implant’s deep threads provide “a large anchoring surface for immediate engaging & stability”. Straumann recommends different drill sequences for soft, medium, and dense bone. For a 4.5mmD Implant in soft bone, a 2.8mmD drill is recommended for final sizing. Forcing an implant into a socket about half its diameter increases the risk of fracturing the bone. Even then, only about half the depth of the apical threads is engaging bone with bone chips filling the void. In medium bone, a 3.7mmD final sizing drill is recommended. This results in only about 1/3 of the depth of the threads engaging bone initially. In dense bone, a 4.2mmD final sizing drill is recommended. This results in only 4.5-4.2/2 = 0.15mm of thread/bone engagement. BLX’s surgical protocol of going back and forth using the bidirectional cutting grooves to fully seat the implant will reduce stability.

The series below shows the narrow and wide abutment options, neither of which achieve a natural emergence profile from the implant’s diameter to the abutment and crown
Below are BLX straight abutments in implants ranging from 3.5mmD to 5.5mmD, and below that are GEN5+™ implants ranging in diameter from 3.3mmD to 5.7mmD with their 1.8mm high friction-fit extenders. NOTE the difference in emergence profile between the two systems.

Straumann acknowledges need for wider abutment but with just one diameter internal conical connection, they need to overlap the implant shoulder with a wider abutment. This sacrifices the stability achieved by engaging the internal conical connection.

The aggressive threads and cutting grooves of the BLX/TLX turn the soft bone into an autogenic bone graft which compromises initial stability. The claw-like effect of the bidirectional cutting grooves. The surgical protocol of using this feature to overcome high insertion torque and allow full seating will decrease initial stability. Below are comments on LinkedIn from Dentists who experienced this dramatic reduction in stability.

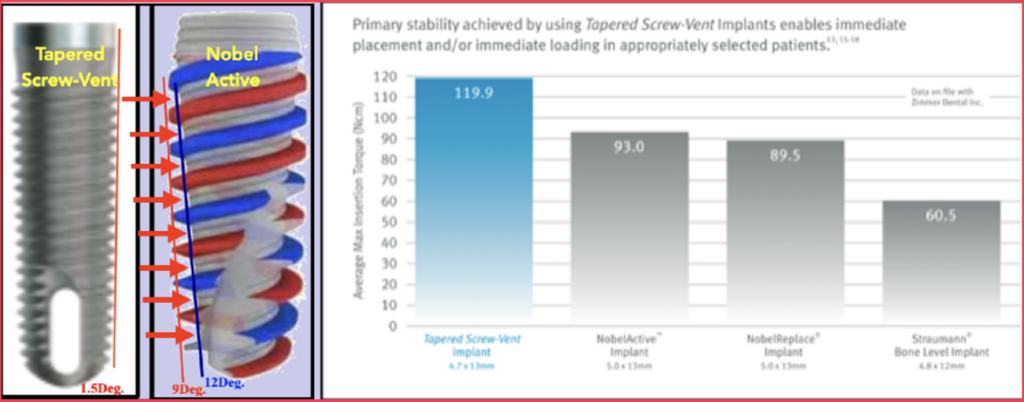
ZimVie’s Torque Tests confirm increasing the depth of the threads actually decreases initial stability. Screw-Vent generated 29% more insertion torque than the NobelActive implant. Niznick 1995 Patent #5,427,527: Dental Implant Method of Installation Niznick G., Article, Oral Health, August 2000: Achieving Osseointegration in Soft Bone:

EVOLUTION AND INNOVATION: THREE PATENTED FEATURES OF THE GEN5™ AND GEN5+™ IMPLANTS


PATENTED FEATURES OF THE 1-PIECE NIZPLANT™ IMPLANT WITH ITS DUAL-FUNCTION PLATFORM


Related Posts

Our mission is to provide high-quality, innovative, dental implants and abutments through internet sales at factory-direct prices.
GET TO KNOW US
LET US HELP YOU
STAY CONNECTED
- Contact Us
- info@paragon-implant.com
- 855.NIZ.GEN5
- Mon-Fri 6am-5pm PST
